‡Percentage of people aged 60─74 year screened for CRC with FIT in 2020/2021
†Percentage of adults aged ≥50 years who had colonoscopy in the past 10 years (2018 data)
¥ Percentage of people screened for CRC with FIT in 12 European Union Member States in 2018
*CRC screening Pilot (2012 – 2017)
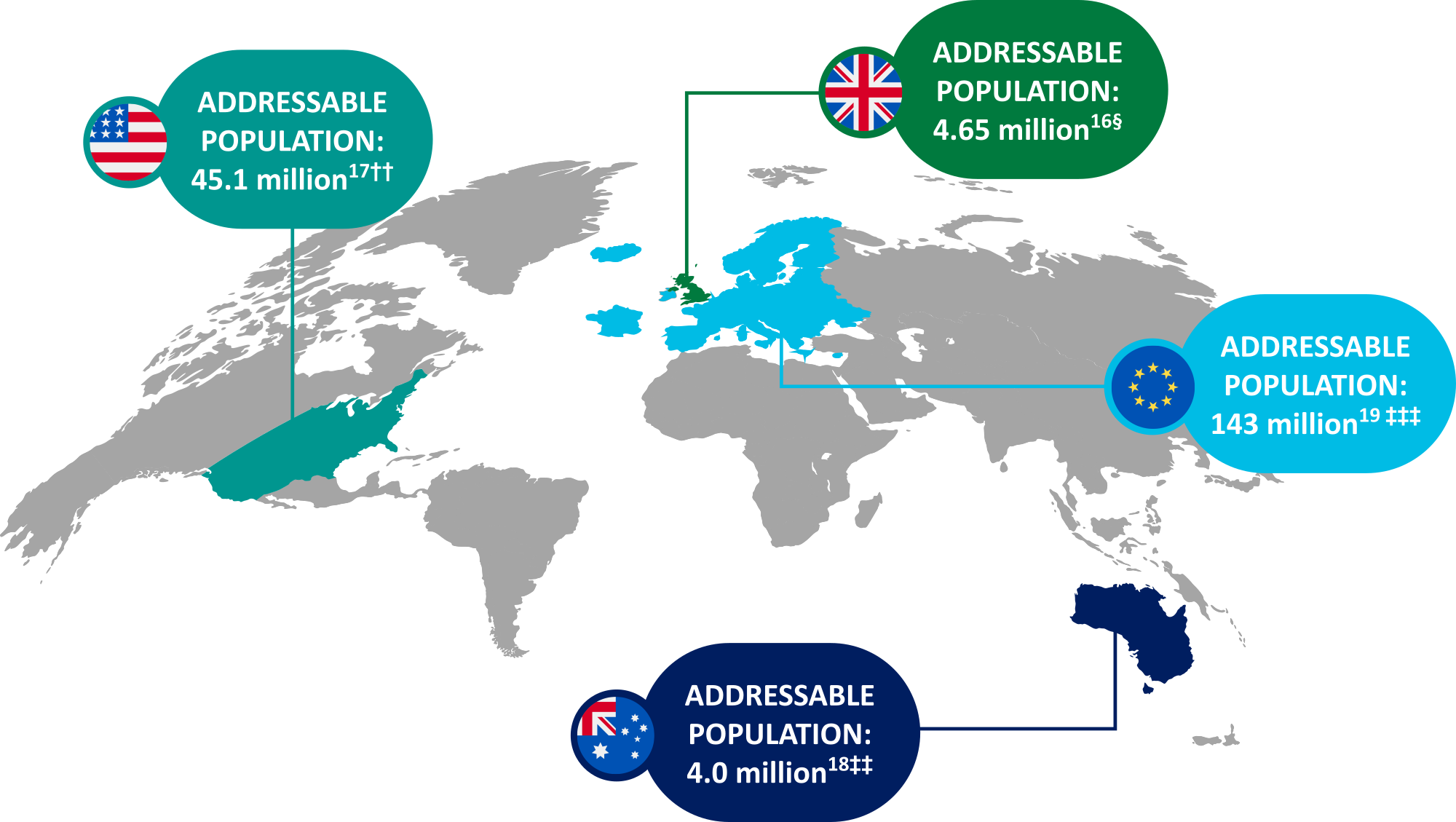
§ Based on 2020 UK population aged 60─74 years of 10,57 million and on 33.2% of the eligible population not being screened for CRC (participation rate: 66.8%).
††Based on 2021 US population aged ≥50 years of 115.62 million and on 39.0% of the eligible population not being screened for CRC (participation rate: 61.0%).
‡‡Based on 2021 Australia population aged 50-74 years of 7.08 million and on 56.5% of the eligible population not being screened for CRC (participation rate: 43.5%).
‡‡‡Based on 2021 Europe population aged 50-74 years of 231 million and on 62% of the eligible population not being screened for CRC (participation rate: 38%).
- Xi Y, Xu P (2021), Global colorectal cancer burden in 2020 and projections to 2040, Translational Oncology, 14(10), 101174,doi:10.1016/j.tranon.2021.101174 Epub 2021 Jul 6
- https://www.cancer.net/cancer-types/colorectal-cancer/risk-factors-and-prevention#:~:text=About%2011%25%20of%20all%20colorectal,cancer%20in%20the%20United%20States
- Colorectal Cancer Statistics | CDC
- Bowel cancer incidence statistics | Cancer Research UK
- Bowel cancer (Colorectal cancer) in Australia statistics | Cancer Australia
- Bowel cancer (Colorectal cancer) in Australia statistics: https://www.canceraustralia.gov.au/cancer-types/bowel-cancer/statistics#:~:text=In%202019%2C%20there%20were%205%2C255,2%2C836%20males%20and%202%2C459%20females)
- Colorectal cancer burden in EU-27. 2020. Available at: https://ecis.jrc.ec.europa.eu/pdf/Colorectal_cancer_factsheet-Mar_2021.pdf
- Hughes et al. J Community Health. Author manuscript; available in PMC 2016 October 25
- American Cancer Society. Colorectal Cancer Facts & Figures 2020-2022. Available at: Colorectal Cancer Facts & Figures 2020-2022
- Office for Health Improvement & Disparities. Cancer service data 2020/2021. Available at: Cancer Services - Data - OHID (phe.org.uk)
- Australia National Bowel Cancer Screening Program: monitoring report 2021. https://www.aihw.gov.au/reports/cancer-screening/nbcsp-monitoring-report-2021/summary
- https://www.health.govt.nz/our-work/preventative-health-wellness/screening/bowel-screening-pilot/bowel-screening-pilot-results#colonoscopies
- Zahnd et al cancer in rural areas US 2018
- nrha-cancer-factsheet-july2022 cancer
- Gordon NP, Green BB. Factors associated with use and non-use of the Fecal Immunochemical Test (FIT) kit for Colorectal Cancer Screening in Response to a 2012 outreach screening program: a survey study. BMC Public Health. 2015 Jun 11;15:546
- UK Office for National Statistics. Interactive population pyramid, mid-2001 to mid-2020. Available at https://www.ons.gov.uk/peoplepopulationandcommunity/populationandmigration/populationestimates/bulletins/annualmidyearpopulationestimates/mid2020. Accessed: 02 November 2022
- US population by age. Statista 2020. Available at: https://www.statista.com/statistics/241488/population-of-the-us-by-sex-and-age/. Accessed: 02 November 2022
- Australian Bureau of Statistics. Population data summary. Available at: Population: Census, 2021 | Australian Bureau of Statistics (abs.gov.au). Accessed: 02 November 2022.
- https://www.statista.com/statistics/253408/age-distribution-in-the-european-union-eu/
- https://bowelcancernz.org.nz/about-bowel-cancer/what-is-bowel-cancer/symptoms-statistics/